By KATHERINE THIBAULT, DPT
By KATHERINE THIBAULT, DPT
Do you have pain in your shoulder and have no idea what could be causing it? Shoulder pain is actually one of the most common reasons people seek out physical therapy. Often times, the rotator cuff is the culprit. The rotator cuff is a group of four muscles: the infraspinatus, supraspinatus, subscapularis and teres minor. Together, these muscles provide stability for the shoulder joint as well as perform rotation of the shoulder. It is a very important muscle group that often wears down over time. The older we get, the more at risk we are for a rotator cuff tear whether it’s from overuse or a traumatic injury.
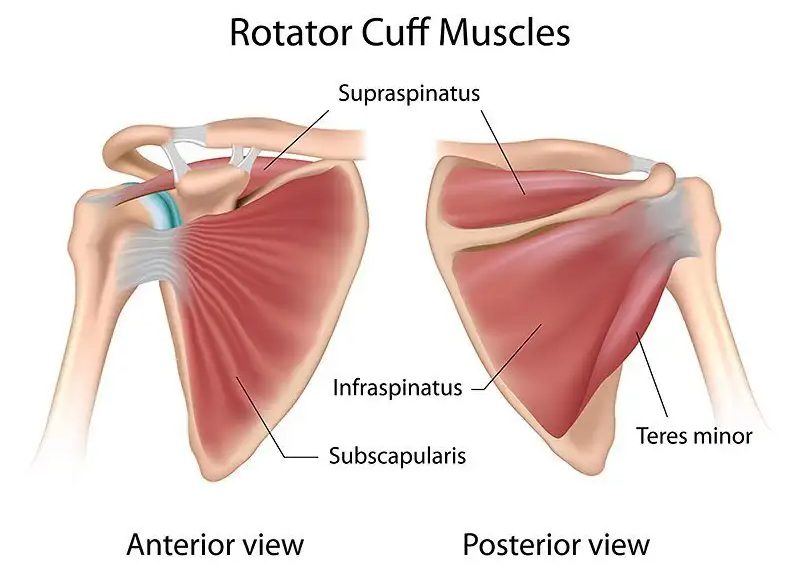
If you are diagnosed with a rotator cuff tear, physical therapy is typically the first line of treatment to work on improving the strength and stability of the shoulder complex. Often times, physical therapy is enough to regain normal function and allow for painless shoulder function. However, depending on the thickness of the tear and number of tendons involved, surgery may be needed. Maybe you’ve gotten to the point where you’ve tried PT and the next step is surgery. You’ve heard dozens of horror stories and are wondering what to expect… keep reading!
The surgical procedure to repair the rotator cuff is typically an arthroscopic surgery with very small incisions. The surgeon will insert an arthroscope, a small camera, which displays the picture onto a television screen and guides the surgeon through the repair. This is typically done as an outpatient procedure and is the least invasive surgical option. The complexity of the repair process will depend on whether the tear is a partial or full tear. If it is a partial tear, the area will be trimmed or smoothed, known as debridement. If it is a full thickness tear, the tendon will need to be reattached to the humeral head. The surgical incisions will be closed with stitches which will usually be removed around week two post-operative at your first follow up visit.
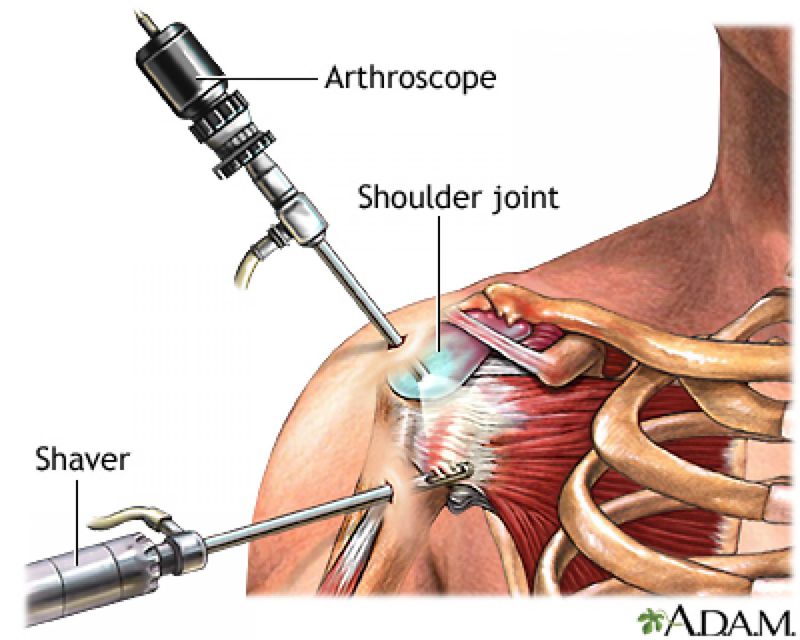
So you’ve gotten through the actual surgery, now what? You will typically be fitted to a sling and will go to your first physical therapy appointment two days post-operative. The sling is usually worn 24/7 for 4-6 weeks and provides protection for your arm while the tendons heal. During your first physical therapy visit, your therapist will remove the surgical dressing and evaluate the passive range of motion of your shoulder joint. Passive range of motion means your therapist will be moving your arm so your tendons and muscles are not contracting, potentially damaging the tendon repair. Each surgeon and protocol varies to some degree but the first few weeks of therapy will consist of your therapist stretching your shoulder passively. The first few weeks of stretching are essential to restore the range of motion of your shoulder. One complication that can occur following surgery is adhesive capsulitis also known as frozen shoulder. This happens when the joint capsule “freezes” and tightens up, usually a result of your shoulder being immobilized in the sling all day. With adhesive capsulitis, restoring full range of motion can be very painful and take much longer. You might feel like you’re not doing much those first few weeks of therapy but being consistent with attendance and allowing your therapist to stretch the joint is essential to ensure full range of motion after surgery.
After the first few weeks of passive stretching, typically around week six, you can begin active range of motion and lifting weight equivalent to a coffee cup. Active range of motion means you are contracting your muscles to move your arm. You are no longer relying on your therapist to perform the motion. Your therapist will guide you through some gentle initial exercises and then begin to add in resistance for strengthening beginning around week 8-12. Together, you and your therapist will work to get you back to full strength and stability allowing your shoulder to withstand daily activities, work duties or athletics. The full rehab process can take 4-6 months or even longer so be patient with the process! Please don’t hesitate to reach out to us at Hampton Physical Therapy for any further questions or concerns regarding a rotator cuff repair.