Physical Therapy Can Help!

By Jessica Leberman, DPT – Hampton Clinic
Medial Tibial Stress Syndrome (MTSS) more commonly referred to as “shin splints” is an injury of the lower leg that primary occurs in the exercising population1. MTSS makes up to 16% of injuries that occur in runners2. MTSS typically presents as pain along the lower 2/3rd of the tibia (shin) bone with activity. Often, the pain is worst immediately upon initiating exercise it then, however, eases as the exercise continues and subsides entirely once stopping exercise. The presentation can vary and as the condition worsens pain at rest can occur.3
What Causes Medial Tibial Stress Syndrome?
As the name indicates, MTSS is a repetitive overuse injury usually affecting runners, dancers and others that participate in athletic-related activities. The pathophysiology of MTSS is thought to be due to periostitis of the tibia that occurs when the tibia is placed under repetitive loading. Biomechanical faults within the lower leg such as specific calf and ankle muscle dysfunction can lead to over-loading/bending the tibia with exercise.3
 Risk Factors of Medial Tibial Stress Syndrome3
Risk Factors of Medial Tibial Stress Syndrome3
- -Elevated Body Mass Index (BMI)
- -Abnormal ankle range of motion
- -Over pronation (flat feet)
- -Abnormal hip range of motion
- -Females > Males
Prevention2
Not all risk factors are completely controllable to prevent MTSS, therefore, it is important to control the factors that can be controlled such as;
- -Proper footwear for exercise
- -Slowly/gradually increasing exercise regimen
- -Avoiding running too much on hard and/or inclined surfaces
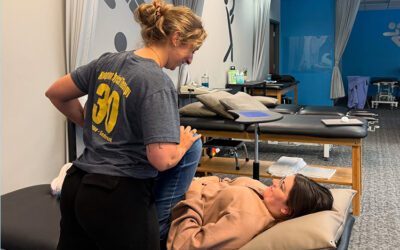
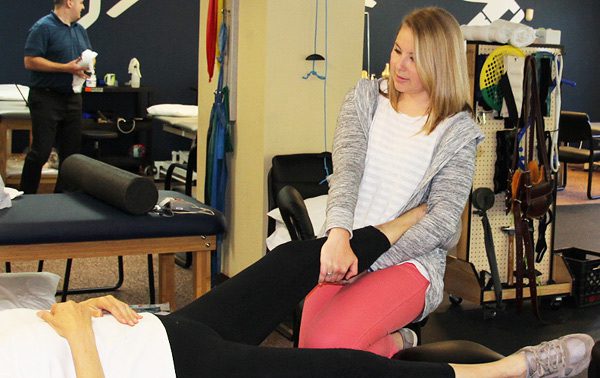 (Dr Jessical Leberman treating a patient with shin splint pain)
(Dr Jessical Leberman treating a patient with shin splint pain)
How Physical Therapy Can Help
The focus of Physical Therapy for MTSS (shin splints) is multifactorial. Initially, soft tissue and joint mobilization manual treatments, stretching, and modalities will be used to reduce inflammation and pain levels and promote healing to the injured area. Guided strength work will be involved to reduce over loading through the tibia. Additionally, your physical therapist will assess foot mechanics to ensure proper footwear is worn to better improve force distribution during exercise. Lastly, your PT will help guide/modify your exercise/training regimen to ensure return to normal activity levels is done correctly to reduce risk of re-injury.3
Contact Hampton Physical Therapy or visit us at www.HamptonPT.com to learn more.
References
1. Winkelmann ZK, Anderson D, Games KE, Eberman LE. Risk Factors for Medial Tibial Stress Syndrome in Active Individuals: An Evidence-Based Review. J AthlTrain. 2016 Dec;51(12):1049-1052
2. Craig DI. Medial tibial stress syndrome: evidence-based prevention. J Athl Train. 2008 May-Jun;43(3):316-8.
3. Galbraith RM, Lavallee ME. Medial tibial stress syndrome: conservative treatment options. Curr Rev Musculoskelet Med. 2009 Oct 7;2(3):127-33.